Charcot foot is a progressive, degenerative condition that affects the joints in the feet and is most commonly associated with vascular complications and nerve damage (neuropathy). Neuropathy is very common among diabetics, making Charcot foot a potential problem for those battling diabetes.
Charcot foot weakens the bones, making them susceptible to fractures. As the condition progresses, the joints collapse and the foot begins to shape itself abnormally. Because of the neuropathy, Charcot foot causes a decrease in the foot’s sensitivity to stimuli and interferes with the muscular balance that controls the foot’s movements.
Often there is no pain, so the person continues walking on the foot—which makes the problem worse.
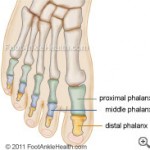
Charcot foot that is left untreated progressively damages the ligaments, cartilage, and bones, and makes the joints in the feet susceptible to progressive injury. It most commonly affects the metatarsal, tarsometatarsal, and midtarsal joints.
All these are located in the forefoot and midfoot. Charcot foot is a very serious condition that can lead to foot deformities, disability, or even amputation.
Charcot foot usually affects only one foot, but 20 percent of patients develop it in both feet. According to the American Diabetes Association, onset of the condition generally occurs after the age of 50, among patients who have been living with diabetes for fifteen years or more.
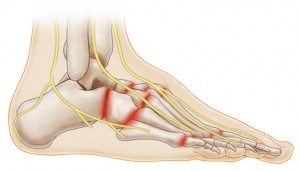
Charcot Foot Symptoms To Know About
Charcot foot is a progressive condition that develops over weeks or months—much faster than peripheral neuropathy, which typically develops over decades. Sometimes a minor trauma may cause the symptoms to appear. Symptoms may include the following:
- Redness
- Swelling
- Pain or soreness
- Warmth within the foot
- Strong pedal pulse
- Instability in the joints
- Loss of sensation in the foot
- Discoloration of the joint
- Subluxation (misalignment of the bones that form a joint)
- Potential nerve damage
- Deformity of the foot (which can be severe)
What Causes Charcot Foot?
If you have been diagnosed with diabetes mellitus and/or peripheral neuropathy, you are at risk of developing Charcot foot. Neuropathy is one of the leading causes of Charcot foot, as it diminishes the patient’s ability to feel pain, temperature, or trauma.
Because of this decrease in sensation, the patient usually does not realize they have the condition. They continue walking on the untreated foot, ultimately causing the condition to worsen. Neuropathic patients who have a tight Achilles tendon are also prone to developing Charcot foot.
Diabetes and hyperglycemia (high levels of glucose in the blood) can trigger neuropathy, which can lead to Charcot foot. How this occurs is still unknown
How Is Charcot Foot Diagnosed?
In order to properly treat Charcot foot, you’ll need to have your symptoms checked out immediately. Catching this condition in its early stages is critical to successful treatment, so you should see a podiatrist at the first sign of symptoms.
Diagnosis can sometimes be difficult because this condition can mimic other conditions like cellulitis or deep venous thrombosis, and because diagnosis of a Charcot fracture cannot be made definitively until bone changes occur.
Therefore traditional methods for early detection (x-rays, MRIs, CT scans, etc) are sometimes not as useful as a nuclear bone scan.
Your foot doctor will need to examine your feet and ask questions about your recent activities, symptoms you are having, and your medical history. X-rays and other imaging tests may be needed to diagnose you properly.
Once the diagnosis is made, you’ll need to have regular exams to keep track of the condition. Your doctor may draw fluid from your joint for laboratory testing to check for fragments of bone and cartilage.
Once you are properly diagnosed, your doctor will create an appropriate treatment plan based on the cause and severity of your condition.
Charcot Foot Treatment Options for You
There are several ways to treat Charcot foot. The main goal is to stabilize the joints. It’s extremely important that you follow the instructions given to you by your foot doctor.
Recovery times can be up to eight weeks or longer, during which time you will be required to stay off your feet. Non-surgical treatment options include:
- Immobilization
- Custom shoes and bracing
- Use of crutches, casts, wheelchair used to protect foot
- Limiting activities that cause the condition
If your condition is severe, or if it has caused severe deformities, surgery may be needed. Your doctor will be able to determine the appropriate surgical procedure for you. An ostectomy is the most common surgical procedure used to treat this condition.
This involves making an incision on the bottom of the foot to remove the abnormal bone growth and bone and cartilage fragments. After an ostectomy, a brace or cast is worn until the foot has completely healed.
Another surgical procedure is a realignment arthrodesis, either to the mid-foot or hindfoot and ankle. During a mid-foot realignment arthrodesis, bony overgrowths are removed and collapsed arches are repaired.
This is done by making an incision in the foot and inserting screws and plates to stabilize the joints and bones.
Patients usually spend one night in the hospital for this procedure, after which they are required to wear a non-weight-bearing cast for three months, followed by a weight-bearing cast for an additional month.
After that, orthotics are used for as long as your doctor thinks necessary. A hind-foot and ankle realignment arthrodesis is identical to the mid-foot procedure except for the recovery period.
Non-weight-bearing casts are required for the first three months after the procedure, and a special brace is worn for an additional two to three months to protect the arch. Braces are custom-made to enable the patient to walk following the surgery.
You should expect to be closely monitored after any of these surgeries to ensure that the problem does not recur. In most cases the patient may resume normal activities after treatment is administered.
What Are the Complications of Charcot Foot?
Charcot foot can cause various complications, including:
- Calluses
- Foot ulcers, especially if the foot is deformed or if the condition is not caught in its early stages
- Bony protrusions (these have potential to become infected if rubbed on the inside of the shoe for an extended period)
- Osteomyelitis (bone infection)
- Inflammation of the joint membranes
- Blood vessel and/or nerve compression
- Loss of sensation in the foot
- Loss of function in the foot
Can Charcot Foot Be Prevented?
As a diabetic patient, you already have plenty of things to worry about, but you play a vital role in preventing Charcot foot. Here are some tips to help you prevent this condition:
- Control your blood sugar levels in order to reduce the progression of nerve damage.
- Get regular check ups with your doctor and podiatrist.
- Check both feet daily for signs of Charcot foot or other related problems.
- Avoid injury to the feet.
Questions to Ask Your Doctor
Here are some questions to ask your doctor about Charcot foot:
- What are the newest treatment methods available?
- Other than my current medical condition, what else can lead to Charcot foot?
- Will a change in my diet help? If so, what nutrients should I be taking?
- What can I change in my home to prevent this condition?
- When can I apply pressure to my foot again?